Thumb ArthritisPainful inflammation
A thumb that's painful, swollen and warm. Stiffness that's worst in the morning and slowly improves once you get going. Joints that flare up unpredictably, sometimes in both thumbs at once.
This pattern is different from wear-based thumb pain. It points to thumb arthritis - inflammation of the thumb joint, often part of a wider inflammatory or autoimmune condition. On this page we explain what it is, how it differs from osteoarthritis, and which treatments are available.
What is thumb arthritis?
Arthritis means inflammation of a joint. With thumb arthritis, the lining of the joint (the synovium) becomes inflamed. This causes swelling, warmth, pain and stiffness. Over time, the inflammation can damage cartilage and bone, leading to deformity and loss of function.
How is this different from CMC arthrosis?
People often confuse the two, but they're separate conditions:
- Arthrosis (osteoarthritis) - mechanical wear of the cartilage. Develops slowly, usually with age. Pain is worse with use.
- Arthritis - inflammation of the joint, often autoimmune. Can develop at any age. Pain is often worse after rest, with morning stiffness.
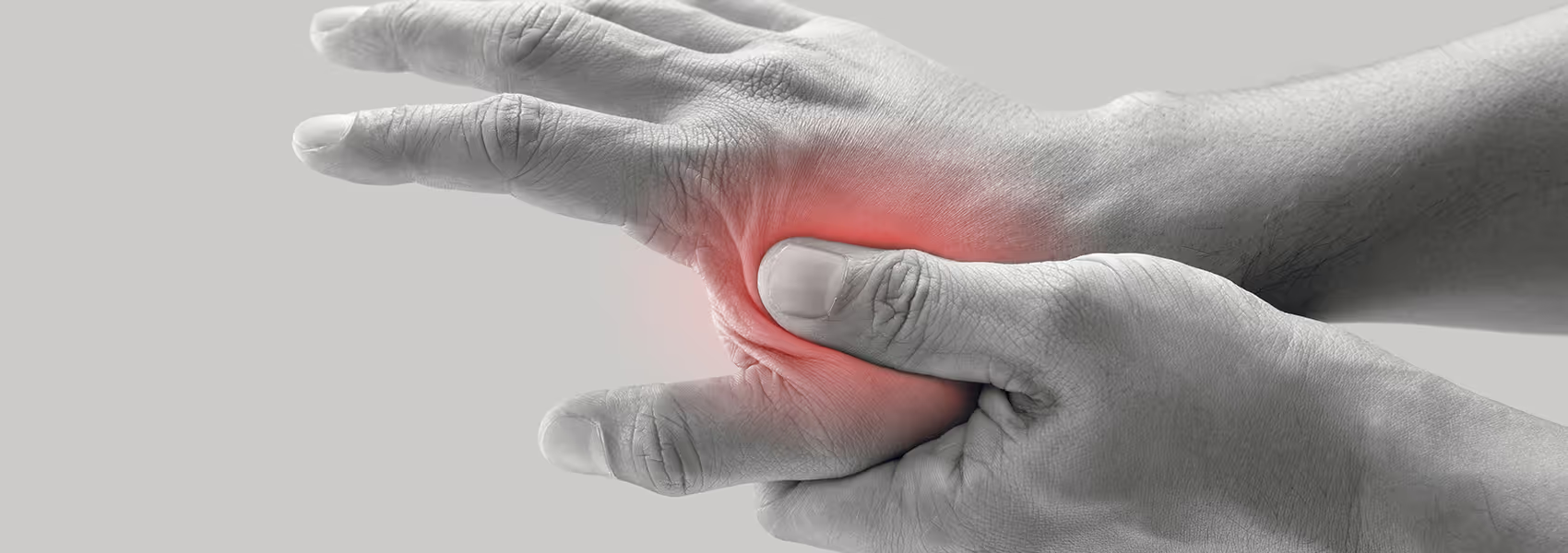
Symptoms of thumb arthritis
Inflammatory thumb arthritis often presents differently from wear-based pain. Typical signs:
- Pain that's worse in the morning or after sitting still, often improving with gentle movement
- Visible swelling around the thumb joint, sometimes with warmth or redness
- Stiffness lasting more than 30 minutes after waking
- Pain that flares up unpredictably and may settle for periods
- Symmetrical involvement — both thumbs or other small joints affected at the same time
- General fatigue or feeling unwell during flare-ups
- Reduced grip strength, especially during active inflammation
What causes thumb arthritis?
Thumb arthritis isn't usually a stand-alone condition. It's often a sign of a broader inflammatory disease:
Rheumatoid arthritis (RA)
The most common cause of inflammatory thumb arthritis. RA is an autoimmune disease where your immune system attacks the joints.
Gout
Caused by uric acid crystals depositing in joints. While gout most commonly affects the big toe, it can also occur in the thumb.
Other autoimmune conditions
Lupus, Sjögren's syndrome and other connective tissue diseases can also cause thumb joint inflammation.
Psoriatic arthritis
An inflammatory arthritis associated with the skin condition psoriasis. It can affect the thumb, often along with the nails and other finger joints.
Reactive arthritis
Inflammation triggered by an infection elsewhere in the body. Usually temporary, but can affect the thumb and other joints.
How is thumb arthritis diagnosed?
Diagnosis usually involves a combination of:
If inflammatory arthritis is suspected, you'll usually be referred to a rheumatologist (a doctor specialising in joint and autoimmune conditions). Early diagnosis matters, inflammation that's left untreated can permanently damage joints.
Treatment of thumb arthritis
Treatment for inflammatory thumb arthritis typically combines medical and supportive approaches. Unlike with arthrosis, medication plays a central role here.

Medical treatment
This is the foundation. A rheumatologist may prescribe:
- DMARDs (disease-modifying antirheumatic drugs): reduce inflammation and prevent joint damage
- Biologics: newer medications that target specific parts of the immune response
- Corticosteroids: for short-term flare control, sometimes by injection into the joint
- NSAIDs: for symptom relief

Hand therapy
A hand therapist can teach you exercises to maintain range of motion, strengthen the muscles around the joint, and protect joints from further damage. Joint protection techniques such as learning how to use your hands in ways that reduce strain are particularly valuable for inflammatory arthritis.

A custom-made brace
Een goed passende brace helpt op meerdere manieren: het rust het gewricht tijdens een opflakkering, ondersteunt de duim zodat je je hand kunt blijven gebruiken, en helpt vervorming te voorkomen. Ook kan het de behoefte aan pijnstilling verminderen.
Bij inflammatoire artritis is maatwerk extra belangrijk. De zwelling varieert van dag tot dag, en een brace die niet goed past kan drukpunten of doorbloedingsproblemen veroorzaken. Een brace op maat past zich aan die veranderingen aan en beschermt het gewricht zonder extra schade te veroorzaken
Discover braces op maat

Surgery
If joint damage from inflammation has become severe and other treatments aren't enough, surgery may be considered. Options include joint fusion (arthrodesis) or joint replacement. Surgery is usually a last resort and works best when the underlying inflammation is well controlled with medication.


Why a custom brace?
Inflammatory arthritis is a serious condition that needs medical treatment. Alongside medication, a custom-made brace could make a real difference to how you function day to day.
How do I know if a brace is a match for me?
Whether a brace is a good treatment for you depends on a few things, and is determined by a medical specialist: where exactly the pain is, how long you've had it, what's causing it, and what you do with your hands during the day. That's different for everyone.
To help you get started, we've created a short online test. You'll answer a few questions about your complaints and then receive an information package tailored to your situation.